Posterior Vitreous Detachment
What is posterior vitreous detachment?
The eye is a very complex functional and anatomic organ. The retina is a thin, delicate and transparent sheet of tissue that lines the inside of the back of the eye. Directly in front of the retina is also a cavity that contains a gel called vitreous, a complex structure consisting of aqueous fluid, macromolecules, and collagen fibrils. In children, the vitreous is an optically clear, transparent, and formed gel. However, as life progresses the vitreous gel naturally and gradually liquifies. By mid to late life, the vitreous has mostly liquified except for a layer of gel up against the retina. At some point, in nearly all people, this layer of gel will spontaneously begin to peel away, or separate, from the retina. We refer to this natural development in the eye as posterior vitreous separation (PVS) or posterior vitreous detachment (PVD).
Posterior vitreous detachment symptoms
The floaters occur because the layer of gel up against the retina contains fibers that clump together when posterior vitreous detachment occurs, then float around within the liquefied vitreous and are symptomatic in the vision. These floaters gradually diminish in prominence over several weeks or months.
Occasionally people will continue to perceive flashes and floaters for a prolonged period of time. As long as a retinal examination discloses no vision-threatening findings, treatment is not necessary.
Risks of leaving PVD untreated
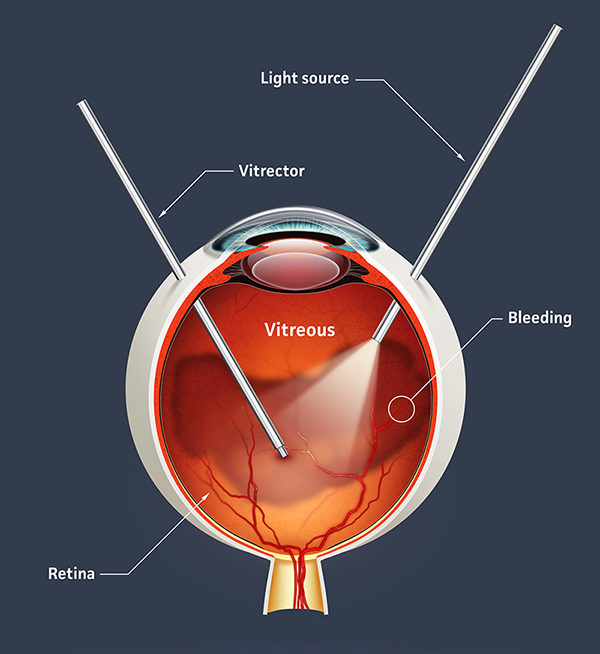
Vision-threatening complications can occasionally develop after a PVS. In some cases, the gel separates from the retina may pull on and break a small retinal blood vessel. This can cause vitreous hemorrhage. Although vitreous hemorrhage will usually resolve on its own, it is also important to examine the retina in case the gel has pulled on the retina hard enough to cause a retinal tear to develop. While laser treatment can help treat & stabilize retinal tears, it can also lead to a retinal detachment which is a very serious and potentially blinding complication of a PVS.
Posterior vitreous detachment treatment
The abrupt onset of flashes and floaters should prompt a careful and complete examination of the back of the eye and the retina within a day or two. Since a retinal tear or retinal detachment may not be initially present, one can occasionally occur later. A second examination is often done 3-4 weeks after the onset of PVS. If we identify no complications at that examination, the future risk is low.
Retina Consultants of Minnesota is a group practice of fellowship-trained Retina Specialists. We specialize exclusively in the treatment of retinal diseases. We are actively involved in research into new treatments and are capable of rapidly bringing newly approved treatments to our patients with retinal diseases.
How long does posterior vitreous detachment take to heal?
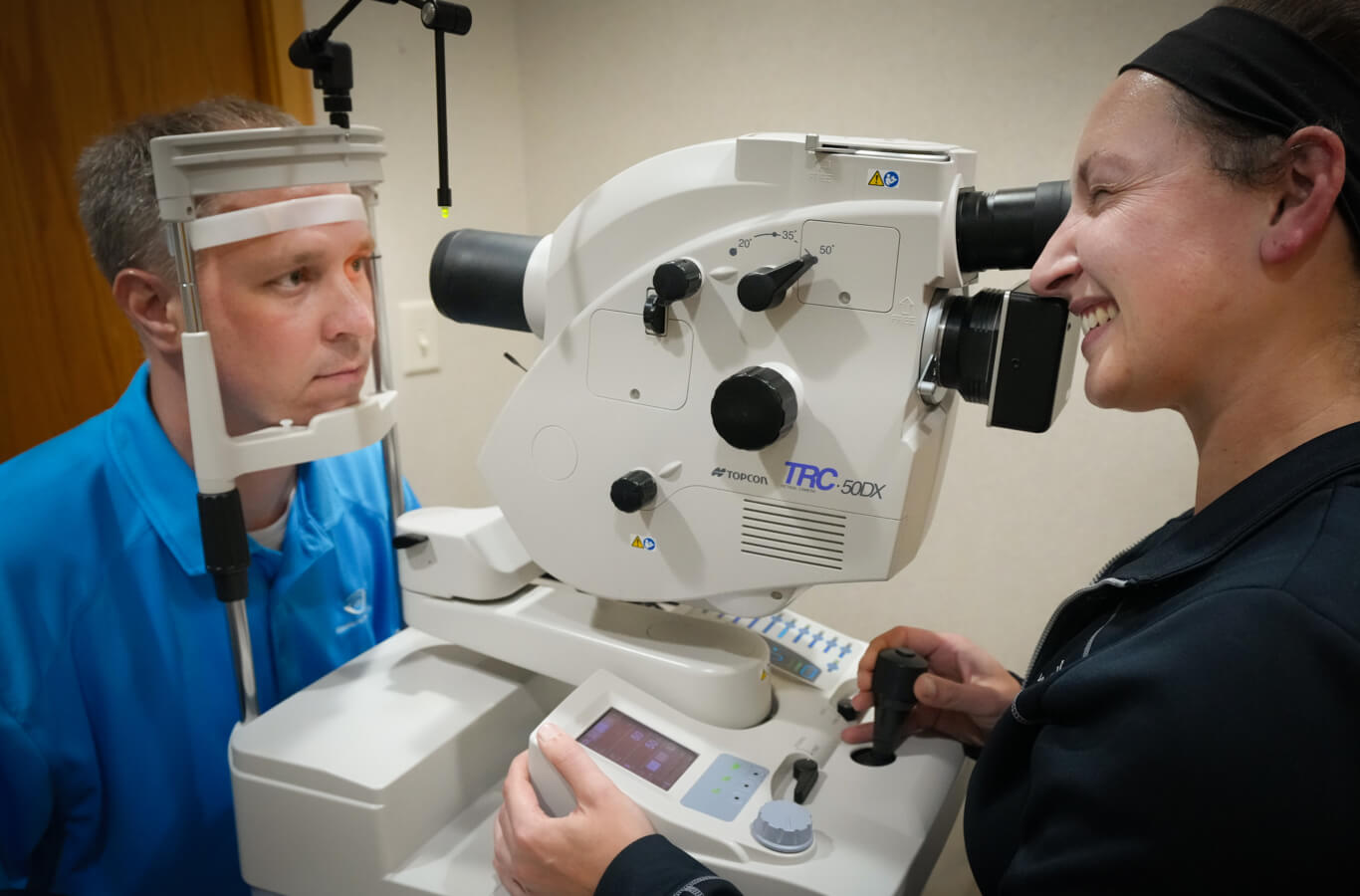
In these cases, the posterior vitreous detachment doesn’t necessarily “heal,” but it doesn’t cause problems for the person’s vision. Floaters or flashes usually get better within three months after determining that there isn’t a retinal tear or detachment.
However, if you notice a lot of floaters or flashes of light suddenly, or if you have a decrease in vision, this demands immediate attention. The retina needs to be examined for a possible retinal tear or retinal detachment. If this has occurred, it is necessary to seal the retina back to the wall of the eye.
This is done with a laser or a freezing procedure. This procedure creates spot welds of sorts around the edges of the tear that nearly eliminates the risk of the tear progressing to full retinal detachment.
If retinal detachment has occurred, we may use a vitrectomy, where we remove the vitreous gel that fills the eye and drain the fluid from under the retina. We then fill the eye interior with a gas bubble to hold the retina in place while it heals. This can also be done with a retinopexy, where a gas bubble is injected into the eye to hold the retina in place to allow it to heal. These procedures will take between 2-4 weeks to heal. It may take longer for your vision to fully return to normal, but most people can return to normal activities.
How common is PVD
Posterior vitreous detachment is completely normal and it occurs in both men and women equally. It most cases it does not require treatment. It doesn’t go away, per se, but the symptoms the patient is experiencing — flashes and floaters — decrease and become less and less noticeable.
Once your eyes are checked to be sure you don’t have either a retinal tear or retinal detachment, usually nothing further is needed.
Is treatment needed?
This is a condition where the vitreous, which was gel when the person was younger, has become liquefied and has begun to peel away from the retina. This is a natural development in the majority of people over the age of 60. It doesn’t heal, but it usually doesn’t require any treatment either.
Who is at risk?
Basically everyone over the age of 60 is at risk for posterior vitreous detachment. Here are the risk factors:
- Older age
- Nearsightedness
- Past eye trauma
- Prior cataract surgery
Schedule a Consultation
To learn more about diabetic retinopathy, please call (855) 515-2020 to schedule a consultation.
We are proud to serve the communities of Minneapolis/St Paul, Brainerd, Duluth, Glencoe, Mankato, St. Cloud, and more.

